About the Client
Our client is a US-based startup that is focused on insurance claims processing automation powered by high-tech machine learning technologies. They also provide customers with task management tools and tailored data-driven recommendations.
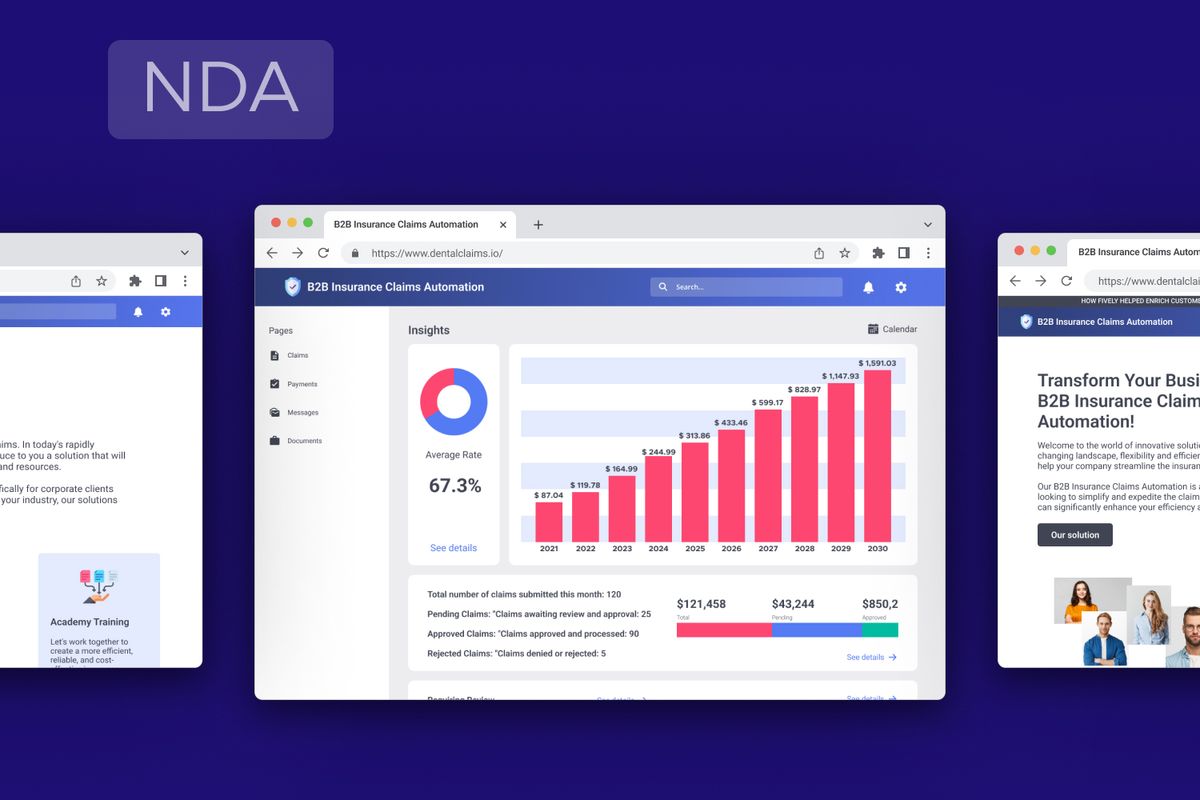
The robotic process automation insurance claims services of our client are widely used by both dental clinics and B2B insurance companies.
Country
the USA
industry
InsurTech
timeline
26 months
team
5-10 developers
Tech stack
80%
of the claims are validated robotically
1.5MM+
claims were processed in 12 months
6 days
is the turnaround time
Fively Reviews
Powered by
THE PROJECT
Custom Software Dev for Dental Insurance Platform
The review
“Our team at Fively is very organized, disciplined, and sharp on timelines.”
Apr 20, 2020
Feedback summary
Fively’s efforts have been met with high praise and appreciation. They’re a welcome addition to the inhouse team and understand the project roadmap well. Customers can expect a team that’s professional, punctual, and communicative.
the project
Custom Software Development
$10,000 to $49,999
Nov. 2019 - Ongoing
PROJECT summary
Fively provides outsourced development services for an insurance startup. They work on internal and external tools using Node.js, Python, and React Native. They also take part in sprint planning.
THE REVIEWER
CEO/Founder, Dental Insurance Platform
Anonymous
Healthcare
San Francisco, California
1-10 Employees
Phone Interview
Verified
Need Help With a Project?
Drop us a line, let’s arrange a discussion
The Challenges of Insurance Claims Processing Automation
Managers of the startup checked in with us to create a top-notch life insurance claims automation services solution for B2B insurance agencies and dental clinics. They chose to go with Fively not only because in San Francisco it was extremely complicated to hire great programmers as quickly as the product roadmap required, but also because they were utterly impressed by our extensive expertise and totally satisfied with our relevant experience.
The main goal of our collaboration was to create a smart tool that will make straight-through processing in insurance a reality. Having completely eliminated any human interaction from the B2B claims handling process, we expected to modernize the customer service, ensure the protection of customer data, and meet even the highest customer demands.
Once we got to work, health insurance claims automation in insurance would never be the same again.
How Fively Helped Enrich Customer Experiences
Insurance companies can quite easily optimize their workflow with a solution devoted to insurance claims processing workflow automation. The ability to maximize time on routine tasks and at the same time track the results of automated processing opens up great opportunities for improving the quality of service and, as a result, improving customer engagement and customer satisfaction rates.
It was the very idea that the founders of the startup came up with. As we see now, they’ve backed the right horse. They also made the right decision, having turned to Fively in order to get a solid technical foundation for their advantageous project.
Finding its niche at the intersection of fintech and healthcare technology, the insurance claim processing services startup has achieved recognition and become a highly sought-after product.
According to the owners of the product, the project can be considered wildly successful. The software for automation in insurance claims handling, developed with the direct involvement of our engineering team, turns out to be very profitable and delights their customers, who in turn trumpet an exceptionally positive user experience.
The Results
Looking back to reflect on the results of several months of work, we can say that we have come up with a non-fungible and really noteworthy tool for the automation of insurance claims in the dental industry.
We've designed and engineered the only dental billing insurance platform that makes the best use of sophisticated machine learning algorithms and AI-driven workflow automation to streamline the insurance revenue cycle management process.
Understanding every little nuance of the future product and paying due attention even to the minor details, we worked not just as an addition, but as part of an in-house development team. However, functioning as a remote software development team, our experts successfully implemented both internal and external tools and backend for those.
Fively's efforts have been met with high praise and appreciation. Customers can expect a team that's professional, punctual, and communicative
Technology Stack For Fintech Automation
Choosing the best tech stack for claim tech solutions development is already half the success. For this particular insurance claims automation solution, it was decided to use the following technologies:
- Typescript
- Apollo GraphQL
- React
- Storybook
- Jest
- Webpack
- Cypress
- Docker
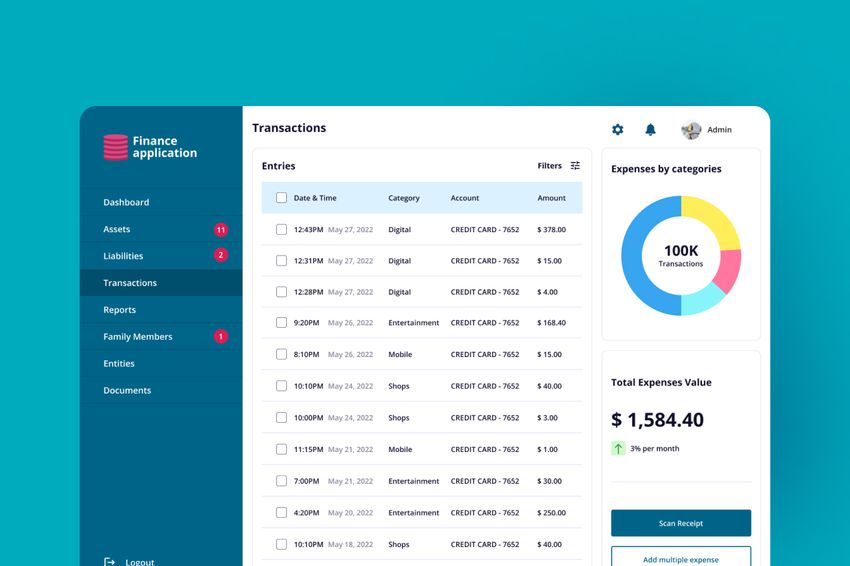
Success Stories
Fively has developed dozens of successful business FinTech products. Make sure to give a closer look at these noteworthy financial technology projects in which our engineers have taken part.
When the insured encounters an accident that falls under the insurance occurrence, they usually apply for an insurance payment that compensates for the losses incurred.
However, the insurance agency must process such a request before allowing the claim and issuing some financial recompense. In the case of health care, requests come from clinics and practices after the patient has received medical care.
When a claim is processed by a human, it not only delays the handling of this request but also introduces a human factor, which adversely affects the quality of performance. If insurance claims are processed for too long, no one will be satisfied with the way things shape up.
In other words, the entire insurance industry is built upon the processing of such requests. Fortunately, there is a solution that can change the rules of the game and heave aside all the obstacles to the flawless and effortless handling of insurance bills.
With every passing day, the importance of the role of modern technologies in business is becoming more and more apparent, and there is hardly anyone who would deny the inevitability of an overwhelming digital transformation in a couple of years.
To a great extent, the task of shaping the future of businesses all across the globe has been imposed on AI and Machine Learning solutions.
In fact, the influence of cutting-edge technologies is highly noticeable even in such a stodgy industry as insurance. For many forward-looking insurance companies, artificial intelligence has become a cornerstone element in the entire insurance workflow automation practice.
Let’s put aside the fact that the integration of AI inevitably reduces costs and increases profits significantly. In many ways, the insurance industry is inextricably linked with insurance claims handling. Nowadays, this monotonous, yet extremely important, claims process can be almost entirely automated.
Thus, a pinch of automation in insurance claims could save the day, becoming a real breakthrough.